Can you live without a bladder
Imagine life without the ability to urinate, holding on to waste until it becomes unbearable, and constantly feeling the urgent need to relieve yourself. This is the reality for people living without a bladder.
Bladder removal, or cystectomy, is a drastic but necessary procedure for those suffering from certain medical conditions. While it may seem impossible to live without this essential organ, advancements in medical technology and surgical techniques have made it possible for individuals to lead fulfilling lives after a cystectomy.
Can You Survive Without a Bladder?
Yes, it is possible to live without a bladder, but it significantly alters one's life and requires significant medical intervention. The bladder's primary function is to store urine produced by the kidneys before its elimination from the body. Removing the bladder, a procedure known as a cystectomy, is typically performed due to bladder cancer, but it can also be necessary for other severe conditions. Living without a bladder necessitates the creation of a new way for urine to exit the body. This is usually achieved through a surgical procedure that creates a urinary diversion. The impact on one's daily life is substantial, requiring adjustments to lifestyle and ongoing medical management.
Types of Urinary Diversion
Several surgical techniques can create a urinary diversion after a cystectomy. The most common include: ileal conduit (where a section of the small intestine is used to create a conduit to drain urine into a stoma on the abdomen), neobladder (where a section of the intestine is reconstructed to create a new bladder), and ureterostomy (where the ureters are diverted directly to the skin). The choice of procedure depends on several factors including the patient's overall health, the extent of the cancer, and surgeon preference. Each method has its own set of advantages and disadvantages regarding continence, complications, and overall quality of life.
Life with a Urinary Diversion
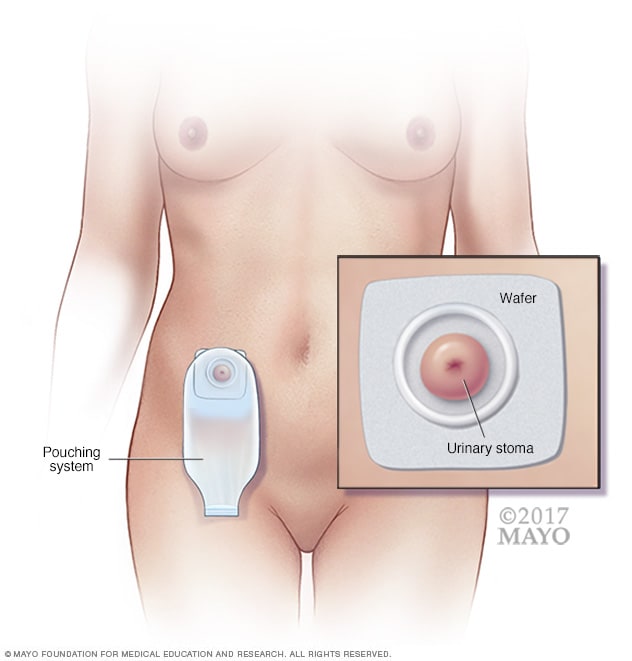
Life after a cystectomy and urinary diversion requires significant adaptation. Patients need to learn how to manage their stoma, including emptying the collection bag regularly and maintaining skin health around the stoma to prevent infection. Depending on the type of diversion, individuals may experience varying degrees of continence. Some diversions allow for more control over urination, while others require the use of an external collection device at all times. Regular medical follow-up is crucial to monitor for complications and ensure proper management of the diversion.
Potential Complications
There are potential complications associated with bladder removal and urinary diversion. These can include infection, kidney stones, stoma issues (such as stenosis or prolapse), and psychological impact adjusting to life with a stoma. Regular check-ups with a healthcare professional are essential to identify and manage any complications that may arise. Proactive management significantly improves the chances of a positive outcome.
Impact on Quality of Life
The impact on quality of life varies widely depending on individual factors, the type of urinary diversion used, and the individual's ability to cope with the changes. Some patients experience a significant reduction in their quality of life due to the challenges of managing a stoma and potential complications. Others successfully adapt and maintain a high quality of life. Emotional support and adequate medical care are crucial to help patients navigate the challenges and adjust to their new reality. Support groups and counseling can significantly improve psychological well-being.
Long-Term Care and Management
Living without a bladder requires long-term medical management. This includes regular check-ups, monitoring for complications, and adjustments to lifestyle to minimize risks. Patients will need to learn how to care for their stoma, manage potential complications, and maintain a healthy lifestyle. Dietary changes may be recommended, and regular exercise, while often challenging, is beneficial for overall health and well-being. Open communication with the healthcare team is essential for optimal long-term management.
| Procedure | Description | Continence | Complications |
|---|---|---|---|
| Ileal conduit | Uses a section of the small intestine to create a conduit draining urine into a stoma. | No | Infection, stoma problems, kidney stones |
| Neobladder | Reconstructs a new bladder from a section of the intestine. | Variable, some continence possible | Infection, leakage, stones |
| Ureterostomy | Directs ureters to the skin surface. | No | Infection, skin irritation |
Can You Survive Without a Bladder?
Yes, it is possible to live without a bladder, but it significantly alters one's life and requires significant medical intervention. The bladder's primary function is to store urine produced by the kidneys before its elimination from the body. Removing the bladder, a procedure known as a cystectomy, is typically performed due to bladder cancer, but it can also be necessary for other severe conditions. Living without a bladder necessitates the creation of a new way for urine to exit the body. This is usually achieved through a surgical procedure that creates a urinary diversion. The impact on one's daily life is substantial, requiring adjustments to lifestyle and ongoing medical management.
Types of Urinary Diversion
Several surgical techniques can create a urinary diversion after a cystectomy. The most common include: ileal conduit (where a section of the small intestine is used to create a conduit to drain urine into a stoma on the abdomen), neobladder (where a section of the intestine is reconstructed to create a new bladder), and ureterostomy (where the ureters are diverted directly to the skin). The choice of procedure depends on several factors including the patient's overall health, the extent of the cancer, and surgeon preference. Each method has its own set of advantages and disadvantages regarding continence, complications, and overall quality of life.
Life with a Urinary Diversion
Life after a cystectomy and urinary diversion requires significant adaptation. Patients need to learn how to manage their stoma, including emptying the collection bag regularly and maintaining skin health around the stoma to prevent infection. Depending on the type of diversion, individuals may experience varying degrees of continence. Some diversions allow for more control over urination, while others require the use of an external collection device at all times. Regular medical follow-up is crucial to monitor for complications and ensure proper management of the diversion.
Potential Complications
There are potential complications associated with bladder removal and urinary diversion. These can include infection, kidney stones, stoma issues (such as stenosis or prolapse), and psychological impact adjusting to life with a stoma. Regular check-ups with a healthcare professional are essential to identify and manage any complications that may arise. Proactive management significantly improves the chances of a positive outcome.
Impact on Quality of Life
The impact on quality of life varies widely depending on individual factors, the type of urinary diversion used, and the individual's ability to cope with the changes. Some patients experience a significant reduction in their quality of life due to the challenges of managing a stoma and potential complications. Others successfully adapt and maintain a high quality of life. Emotional support and adequate medical care are crucial to help patients navigate the challenges and adjust to their new reality. Support groups and counseling can significantly improve psychological well-being.
Long-Term Care and Management
Living without a bladder requires long-term medical management. This includes regular check-ups, monitoring for complications, and adjustments to lifestyle to minimize risks. Patients will need to learn how to care for their stoma, manage potential complications, and maintain a healthy lifestyle. Dietary changes may be recommended, and regular exercise, while often challenging, is beneficial for overall health and well-being. Open communication with the healthcare team is essential for optimal long-term management.
| Procedure | Description | Continence | Complications |
|---|---|---|---|
| Ileal conduit | Uses a section of the small intestine to create a conduit draining urine into a stoma. | No | Infection, stoma problems, kidney stones |
| Neobladder | Reconstructs a new bladder from a section of the intestine. | Variable, some continence possible | Infection, leakage, stones |
| Ureterostomy | Directs ureters to the skin surface. | No | Infection, skin irritation |
Can you survive without a bladder?
Yes, you can survive without a bladder. However, it's not a simple matter of just removing it and expecting to live a normal life. The bladder's primary function is to store urine produced by the kidneys. Without a bladder, a surgical procedure called urinary diversion is necessary. This involves creating a new way for urine to exit the body. There are several different types of urinary diversions, each with its own set of advantages and disadvantages. These procedures can be quite complex and involve significant recovery time. While it's possible to live a relatively normal life after a urinary diversion, there will be noticeable changes to your daily routine. These changes might include the need for frequent catheterization or the use of an external collection device. The specific challenges will depend on the type of diversion surgery performed and the individual's overall health. Ultimately, living without a bladder requires careful management and adaptation, but it is certainly possible.
What are the consequences of living without a bladder?
Living without a bladder inevitably brings about significant changes to one's life. The most immediate consequence is the need for a urinary diversion, as mentioned earlier. This means that urine will no longer be stored in a bladder but will be diverted through a different pathway. Depending on the chosen surgical procedure, this could involve several potential complications. These might include frequent infections, the need for ongoing medical care, and the possibility of complications related to the surgery itself. Furthermore, individuals may experience changes in their body image and lifestyle adjustments. The need for regular catheterization, wearing an external collection device, or managing an internal reservoir can be physically demanding and emotionally challenging. The long-term effects can also include potential kidney damage if the diversion is not properly managed. The severity of these consequences varies widely based on factors like the individual's overall health, the type of urinary diversion, and the quality of post-operative care.
What are the different types of urinary diversion surgeries?
There are various surgical options for creating a urinary diversion, each with its own pros and cons. Ileal conduit is a common procedure where a segment of the ileum (small intestine) is used to create a conduit that carries urine from the kidneys to a stoma (an opening on the abdomen). This requires an external collection device. Continent urinary reservoir surgeries create a pouch within the body to store urine, usually from a segment of the bowel. This reduces the need for external devices, but it necessitates regular catheterization to empty the reservoir. Neobladder surgery creates a new bladder from a section of the bowel, allowing for natural urination in some cases. However, this may not always be fully successful, and some individuals may still need catheterization. The choice of surgery is determined by several factors, including the patient's overall health, the cause of bladder removal, and their preferences. It's crucial to discuss all the options thoroughly with a urologist to make an informed decision that best suits one's individual needs and circumstances.
What is the recovery process like after bladder removal surgery?
The recovery process following bladder removal and urinary diversion surgery is lengthy and complex. It involves a significant period of hospitalization followed by several weeks or even months of recovery at home. The initial phase involves managing pain, healing from the surgery, and adjusting to the new urinary system. Pain management is crucial, and patients are typically given medication to alleviate discomfort. Learning to care for the stoma (if applicable) or managing catheterization is a significant part of the recovery process. This often requires specialized training from nurses and healthcare professionals. The recovery period also includes adjusting to lifestyle changes that come with managing a urinary diversion. This can involve diet modifications, regular monitoring of urine output and stoma health, and potential ongoing medical appointments. Physical and occupational therapy may be necessary to help regain strength and mobility. The emotional impact of the surgery should not be overlooked, and support groups or counseling can be invaluable during this challenging time. The entire process requires patience, dedication, and a strong support system.
Deja una respuesta