Does fasting heal cells
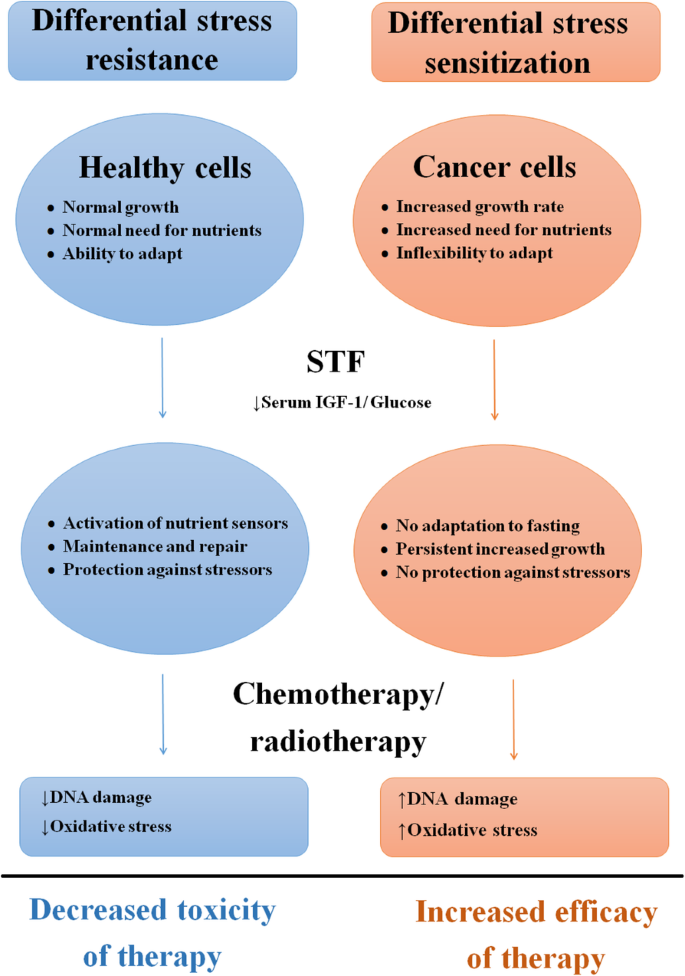
Fasting, a practice that involves voluntarily abstaining from food for a period of time, has been gaining increasing attention for its potential health benefits. While fasting has been traditionally used for religious and spiritual purposes, modern research is uncovering its potential role in cellular rejuvenation and healing. In this article, we delve into the intriguing question: "Does fasting heal cells?" We explore the latest scientific findings, examining how fasting impacts cellular processes, promotes autophagy, and potentially reduces inflammation and oxidative stress. By delving into the complex interactions between fasting and cellular health, we aim to provide evidence-based insights into the potential of fasting as a therapeutic tool for promoting cellular rejuvenation and overall well-being.
Does Fasting Heal Cells? Exploring the Cellular Benefits of Intermittent Fasting
The question of whether fasting heals cells is complex and not definitively answered with a simple yes or no. While there's growing evidence suggesting fasting can positively impact cellular health, it's not a miracle cure and its effects depend heavily on various factors, including the type of fasting, duration, individual health, and overall lifestyle. The mechanisms through which fasting might promote cellular healing are primarily related to its ability to trigger cellular processes like autophagy and reduce inflammation. However, more research is needed to fully understand the extent and limitations of fasting's cellular benefits.
Cellular Autophagy: A Cleaning Process
One of the key ways fasting may contribute to cellular healing is through autophagy. This is a natural cellular process where damaged cells, proteins, and organelles are broken down and recycled. Think of it as the cell's own built-in cleaning and recycling system. During periods of fasting, when nutrient intake is restricted, the body initiates autophagy to conserve energy and eliminate cellular debris. By removing damaged components, autophagy helps to maintain cellular health and function. This process can be particularly important in mitigating the effects of aging and preventing the accumulation of cellular damage linked to various diseases.
Reduced Inflammation: A Key Factor in Healing
Chronic inflammation is implicated in many diseases, from heart disease to cancer. Studies suggest that fasting can have anti-inflammatory effects. By reducing inflammation, fasting may create a more favorable environment for cellular repair and regeneration. The mechanisms behind this anti-inflammatory effect are still being explored, but they likely involve changes in the production of inflammatory cytokines and other signaling molecules. This reduction in inflammation may support overall cellular health and potentially aid in the healing process.
Stem Cell Activity: Regeneration and Repair
Some research suggests that fasting might influence the activity of stem cells. Stem cells are undifferentiated cells capable of differentiating into various specialized cell types. By stimulating stem cell activity, fasting could potentially promote tissue repair and regeneration. This is a relatively new area of research, and more investigation is needed to understand the precise mechanisms and the extent to which fasting influences stem cell behavior. However, the potential implications for tissue repair and cellular rejuvenation are significant.
Mitochondrial Function: Energy Production and Cellular Health
Mitochondria are the powerhouses of cells, responsible for generating energy. Studies indicate that fasting can improve mitochondrial function. This enhancement in energy production can be crucial for cellular health and repair processes. Improved mitochondrial function can contribute to overall cellular efficiency and help cells better cope with stress and damage. This is also a complex area of research, however, the benefits of healthier mitochondria are undeniable for cellular repair and regeneration.
Cellular Senescence: Slowing Down Aging
Cellular senescence refers to a state where cells stop dividing but don't die, often accumulating damage that can contribute to aging and disease. Some preliminary research suggests that fasting might influence cellular senescence by either removing senescent cells or inhibiting their detrimental effects. This is a promising area of research, but further investigation is necessary to confirm these findings and fully elucidate the mechanisms involved.
| Process | Effect on Cellular Healing |
|---|---|
| Autophagy | Removes damaged cellular components, promoting cellular cleanup and rejuvenation. |
| Reduced Inflammation | Creates a more favorable environment for tissue repair and regeneration. |
| Stem Cell Activity | Potentially stimulates tissue repair and regeneration. |
| Mitochondrial Function | Enhances energy production, crucial for cellular health and repair. |
| Cellular Senescence | May slow down the accumulation of cellular damage associated with aging. |
Is fasting good for cell repair?

Whether fasting is good for cell repair is a complex question with no simple yes or no answer. The effects of fasting on cellular processes are multifaceted and depend on several factors, including the type of fasting (intermittent fasting, prolonged fasting, etc.), the duration of the fast, the individual's overall health, and their genetic predisposition. While some studies suggest potential benefits for cellular repair through processes like autophagy, other research highlights potential risks and limitations. It's crucial to understand that the research is ongoing, and more studies are needed to fully elucidate the relationship between fasting and cell repair.
Autophagy and Cellular Cleanup
Autophagy is a cellular process that involves the breakdown and recycling of damaged components within cells. Fasting triggers autophagy, potentially leading to the removal of dysfunctional organelles and proteins, thereby promoting cellular health. This process is crucial for removing cellular debris that can contribute to aging and disease. However, the extent to which fasting enhances autophagy and subsequently improves cell repair varies significantly.
- Increased Autophagy: Fasting leads to an increase in autophagic flux, effectively clearing out damaged cellular components.
- Improved Mitochondrial Function: Autophagy helps to remove damaged mitochondria, improving overall cellular energy production.
- Reduced Cellular Stress: By removing cellular debris, autophagy decreases cellular stress and promotes a healthier cellular environment.
Cellular Regeneration and Stem Cells
Some studies suggest that fasting may stimulate the production of new cells and enhance the function of stem cells. Stem cells are crucial for tissue repair and regeneration, and their activity is influenced by various metabolic factors, including those altered by fasting. This potential benefit is linked to the body's need to conserve energy during fasting, leading to changes in cellular signaling pathways that might positively impact stem cell activity. More research is necessary to fully understand the mechanism and extent of this effect.
- Stimulation of Stem Cell Proliferation: Fasting may trigger the multiplication of stem cells, leading to a greater capacity for tissue repair.
- Enhanced Stem Cell Differentiation: Fasting might influence the differentiation of stem cells into specific cell types needed for tissue repair.
- Improved Tissue Regeneration: An increase in functional stem cells could enhance the body’s ability to repair and regenerate damaged tissues.
Inflammation and Oxidative Stress
Chronic inflammation and oxidative stress are major contributors to cellular damage and aging. Some research indicates that fasting may help reduce inflammation and oxidative stress, thus indirectly supporting cell repair. However, the effects on inflammation are complex and can vary depending on factors like the duration and type of fasting, and the individual's health status. Further investigation is needed to fully characterize the relationship between fasting, inflammation, and cellular repair.
- Reduced Inflammatory Markers: Fasting can lower levels of inflammatory cytokines, proteins that contribute to inflammation.
- Improved Antioxidant Defense: Fasting may enhance the body's ability to combat oxidative stress through the production of antioxidants.
- Decreased Oxidative Damage: Reduction of oxidative stress can minimize damage to cellular components and DNA.
DNA Repair and Cellular Senescence
Cellular senescence, or the aging of cells, is associated with reduced DNA repair capacity. The impact of fasting on DNA repair mechanisms is not yet fully understood. While some preclinical studies suggest potential positive effects, more research is needed to determine if and how fasting might improve DNA repair efficiency and delay cellular senescence. It’s crucial to consider that any benefit may be indirect or limited to specific types of cellular damage.
- Potential Enhancement of DNA Repair Pathways: Fasting may indirectly stimulate DNA repair pathways, but more research is needed.
- Delayed Cellular Senescence: Some studies suggest a possible delay in cellular aging, though this requires further investigation.
- Limited Direct Effects: The impact of fasting on DNA repair mechanisms might be indirect and dependent on other cellular processes.
Individual Variability and Potential Risks
It's important to emphasize that the effects of fasting on cell repair are highly individualized. Factors such as age, underlying health conditions, genetic predisposition, and the type and duration of fasting all influence the outcome. Furthermore, improper fasting can lead to several negative consequences, including nutrient deficiencies, muscle loss, and metabolic imbalances. Therefore, it's crucial to consult a healthcare professional before embarking on any fasting regimen, especially if you have pre-existing health conditions.
- Nutrient Deficiencies: Improper fasting can lead to deficiencies in essential vitamins and minerals.
- Muscle Loss: Prolonged fasting can result in the breakdown of muscle tissue.
- Metabolic Imbalances: Disruptions in metabolic processes can occur if fasting is not managed properly.
How long do you need to fast to regenerate cells?
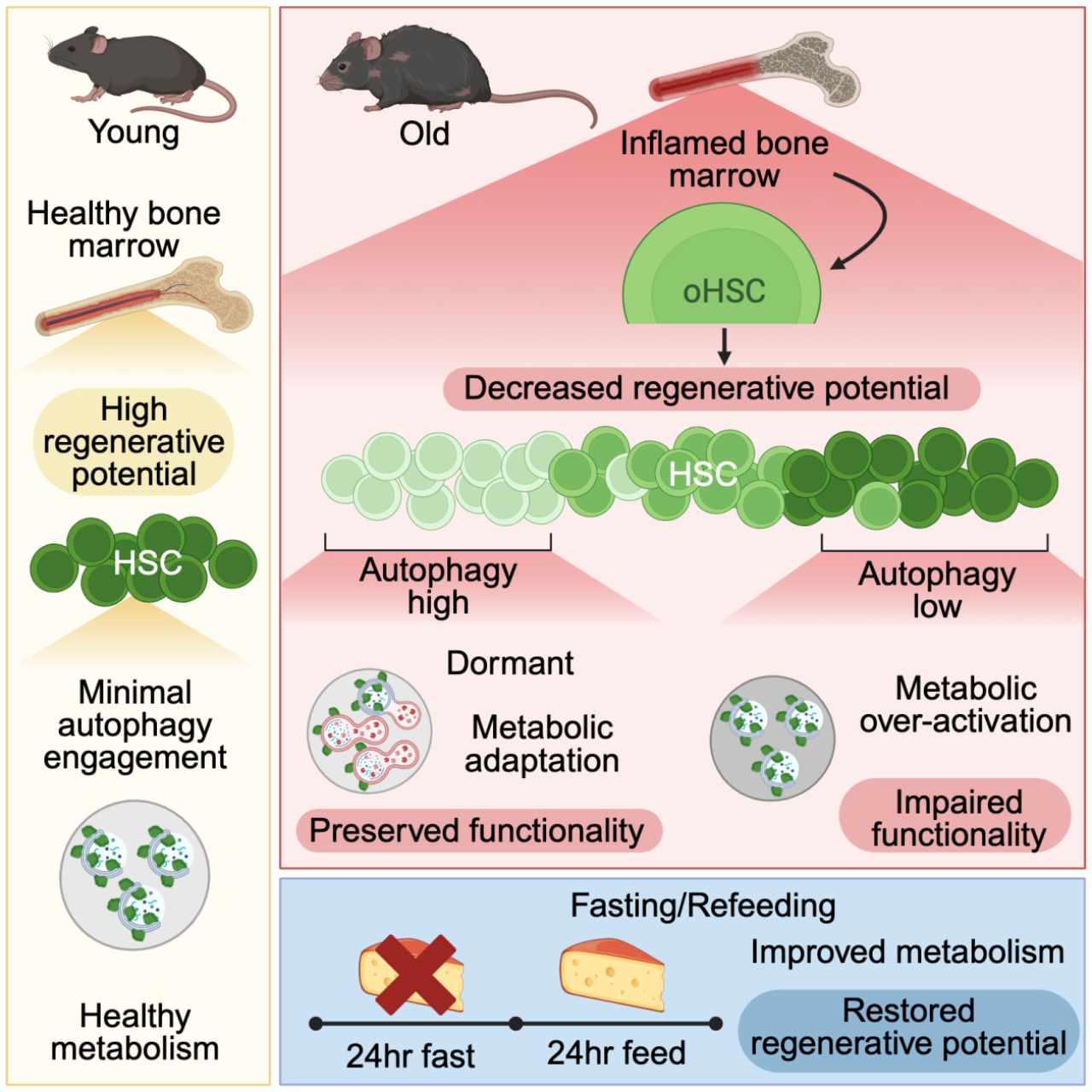
There's no single answer to how long you need to fast to regenerate cells. The process of cellular regeneration is complex and depends on many factors, including your age, overall health, the type of cells being considered, and the extent of damage needing repair. There's no magic fasting duration that universally triggers significant cellular regeneration. While fasting can trigger certain cellular processes that contributeto regeneration, it's not a direct, immediate cause-and-effect relationship. Research suggests that some benefits may be seen even with shorter fasts (e.g., intermittent fasting), while others might require longer periods of fasting.
What types of cells regenerate during fasting?
Fasting primarily impacts cellular processes related to autophagy and apoptosis. Autophagy is the process by which cells break down and recycle damaged components, while apoptosis is programmed cell death, which is essential for removing damaged or unhealthy cells. These processes don't regenerate allcells; rather, they contribute to the body's overall cellular health by eliminating damaged cells and clearing space for new ones. This is particularly evident in immune system cells. Not all cells regenerate at the same rate, or even at all.
- Immune System Cells: Fasting can influence the production and activity of immune cells, potentially leading to improved immune function. This doesn't mean entire organs are regenerated, but rather, their cellular components are renewed and replaced.
- Stem Cells: While fasting doesn't directly trigger the creation of new stem cells, it can create an environment more conducive to their activity and proliferation. However, this process is still incompletely understood and requires further research.
- Specific Tissues: The regeneration of tissues like liver, skin and gut lining cells can be indirectly influenced. For instance, the liver, known for its regenerative capacity, may show improved function after a period of fasting, as the damaged cells are removed and the healthy ones are better supported.
How does fasting influence cellular regeneration?
Fasting triggers several metabolic shifts. It reduces the body's reliance on glucose and promotes the breakdown of stored fats (ketosis). This metabolic change can lead to increased autophagy, and a reduction in inflammation. These processes indirectly support cellular repair and renewal, though the direct impact on the regeneration of specific cell types needs more detailed study. Reduced inflammation is particularly relevant as chronic inflammation can impede regeneration.
- Autophagy Enhancement: Fasting promotes autophagy, the cellular "self-cleaning" process that removes damaged organelles and proteins.
- Reduction in Inflammation: Lowered inflammation creates a more favorable environment for cell repair and regeneration.
- Stem Cell Activity: While not fully understood, studies suggest fasting may indirectly support stem cell activity, although this area needs further exploration.
What are the potential risks of prolonged fasting?
Prolonged fasting, particularly without proper medical supervision, can carry several risks. These include muscle loss, electrolyte imbalances, and nutrient deficiencies. Individuals with pre-existing health conditions should avoid prolonged fasting without consulting their doctor. Fasting should always be undertaken responsibly and in consultation with healthcare professionals.
- Nutrient Deficiencies: Prolonged fasting can lead to a lack of essential nutrients.
- Muscle Loss: The body may start breaking down muscle tissue for energy if fasting is too prolonged or improperly managed.
- Electrolyte Imbalances: Imbalances in electrolytes such as sodium and potassium can be dangerous.
What research supports the connection between fasting and cellular regeneration?
Research on fasting and cellular regeneration is ongoing. Studies in animals have shown promising results, with autophagy and other cellular processes being significantly affected by fasting. However, translating these findings directly to humans is challenging. Human studies are needed to definitively establish the optimal duration and benefits of fasting for cellular regeneration, and many more clinical trials are required to confirm the observed effects.
- Animal Studies: Multiple animal studies demonstrate the positive effects of fasting on autophagy and cellular processes related to regeneration.
- Human Observational Studies: Some observational studies in humans have shown correlations between intermittent fasting and markers of improved cellular health, but these are not definitive proof of causation.
- Ongoing Clinical Trials: Research continues to investigate the long-term effects and optimal protocols for fasting to promote cellular regeneration in humans.
What are the different types of fasting and their potential impact on cellular regeneration?
Various fasting methods exist, including intermittent fasting (such as the 16/8 method or 5:2 diet), water-only fasting, and prolonged fasting. The type of fasting may influence the extent of cellular changes. The effects may vary depending on the duration, frequency, and the individual's response. More research is needed to understand which type, if any, is optimal for promoting cell regeneration.
- Intermittent Fasting (IF): This involves cycling between periods of eating and voluntary fasting, often on a daily or weekly basis. This is the most widely studied type of fasting regarding health and cellular regeneration.
- Prolonged Fasting: This involves abstaining from food for extended periods, often under medical supervision. It can lead to more significant metabolic shifts, but also carries greater risk.
- Specific Dietary Restrictions: Some fasting protocols incorporate specific dietary restrictions, further modifying the metabolic response and impact on cell regeneration.
Does fasting get rid of damaged cells?
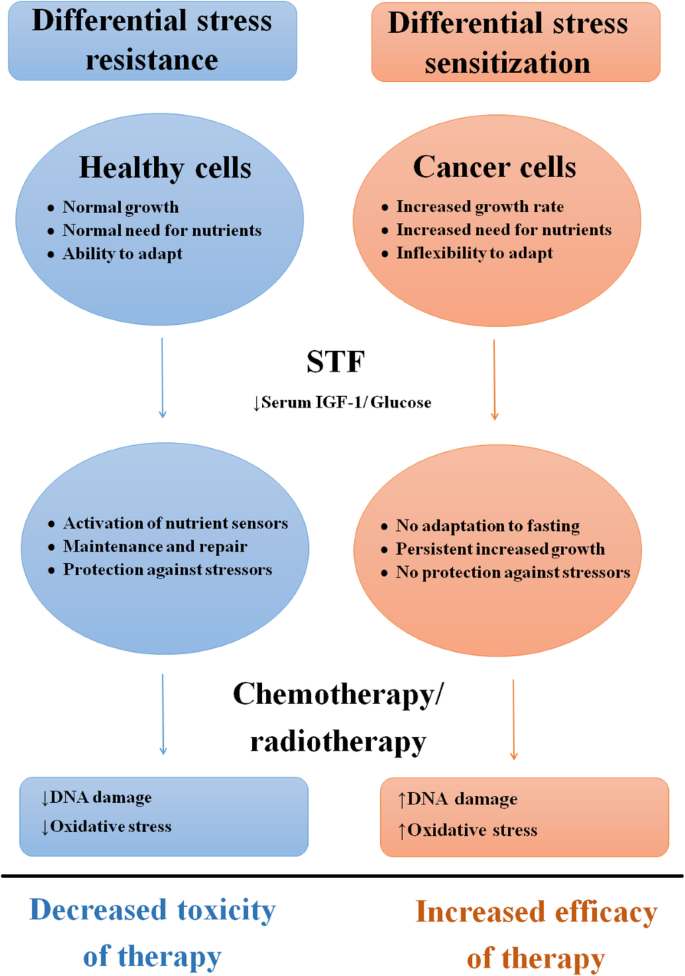
No, fasting does not directly get rid of damaged cells. While fasting triggers several cellular processes that can indirectly benefit cellular health and potentially reduce the numberof damaged cells over time, it doesn't actively target and remove them. The removal of damaged cells is primarily handled by the body's natural processes of apoptosis (programmed cell death) and autophagy (a process of cellular self-cleaning). Fasting can enhanceautophagy, but it doesn't replace it.
How Fasting Impacts Cellular Processes
Fasting primarily influences cellular processes indirectly. It doesn't directly remove damaged cells, but it can create an environment more conducive to cellular repair and renewal. Autophagy, a critical cellular cleaning process, is significantly enhanced during fasting. This process helps to remove damaged organelles and proteins within cells. This improved cellular cleaning can indirectly lessen the burden of damaged cells. Additionally, fasting can reduce inflammation, which is often associated with cellular damage.
- Reduced inflammation: Fasting can lower levels of inflammatory markers, potentially reducing the damage caused by inflammation.
- Enhanced autophagy: This process cleans out damaged components within cells, making way for healthier cellular functions.
- Improved cellular function: By removing damaged parts and reducing inflammation, fasting can help existing healthy cells function more efficiently.
Autophagy and Cellular Clean-Up
Autophagy is a key cellular process that plays a crucial role in removing damaged components within cells. During autophagy, the cell essentially recycles its own components, breaking down damaged organelles, proteins, and other cellular debris. Fasting significantly upregulates autophagy, potentially leading to a reduction in the number of damaged cells over time. However, it's important to understand that this is an indirect effect; fasting doesn't directly target and eliminate damaged cells.
- Cellular self-cleaning: Autophagy is the cell's internal recycling system, removing damaged parts.
- Enhanced by fasting: Fasting significantly boosts the activity of autophagy.
- Indirect effect on damaged cells: While it doesn't directly remove them, it reduces the accumulation of damage.
The Role of Apoptosis in Cell Turnover
Apoptosis, or programmed cell death, is another crucial process involved in eliminating damaged or dysfunctional cells. It is a controlled mechanism that prevents the accumulation of damaged cells that could harm the organism. While fasting doesn't directly trigger apoptosis, some research suggests it may indirectly influence this process. This indirect influence could contribute to a decrease in the overall number of damaged cells. However, apoptosis is a tightly regulated process and is not solely influenced by fasting.
- Programmed cell death: Apoptosis is a controlled mechanism for eliminating damaged cells.
- Tightly regulated: This process is carefully controlled and not directly manipulated by fasting.
- Indirect influence: Fasting's influence on apoptosis is likely indirect and requires further research.
The Limitations of Fasting in Cellular Repair
It's crucial to understand that fasting is not a cure-all for cellular damage. While it can enhance cellular processes that contribute to cellular health, it doesn't directly remove damaged cells. Severe cellular damage, such as that caused by certain diseases or injuries, may not be significantly impacted by fasting alone. Furthermore, prolonged or improperly executed fasting can have negative consequences for health.
- Not a direct removal method: Fasting does not directly target and remove damaged cells.
- Limitations in severe damage: It may not be effective for significant or irreversible cellular damage.
- Potential negative consequences: Improper fasting can harm health; expert guidance is recommended.
The Importance of a Holistic Approach
Maintaining overall health involves a multifaceted approach. While fasting can be a beneficial component of a healthy lifestyle for some individuals, it shouldn't be considered a standalone solution for addressing cellular damage. A balanced diet, regular exercise, adequate sleep, and stress management are all crucial for promoting cellular health and mitigating cellular damage. Combining fasting with these other healthy lifestyle choices may yield more significant benefits than fasting alone.
- Holistic approach: Cellular health requires a comprehensive strategy, not just fasting.
- Lifestyle factors matter: Diet, exercise, sleep, and stress management all play key roles.
- Synergistic effects: Combining fasting with other healthy habits may amplify benefits.
What does fasting do to your cells?

What Does Fasting Do to Your Cells?
Fasting initiates a complex cascade of cellular changes, primarily driven by the body's shift from a fuel-rich to a fuel-scarce state. When nutrient intake ceases, the body begins to utilize stored energy reserves. This process affects cellular function in several significant ways, impacting metabolism, repair, and even cellular lifespan. The specific changes depend on the duration and type of fast (intermittent vs. prolonged), individual factors like age and health status, and the cell type itself. Cellular responses to fasting are highly dynamic and intricate, involving multiple signaling pathways and molecular mechanisms. Research is ongoing, constantly revealing new facets of this complex interplay.
Cellular Autophagy
Autophagy, meaning "self-eating," is a crucial cellular process significantly upregulated during fasting. It involves the degradation and recycling of damaged or dysfunctional cellular components. This cellular cleanup process is vital for removing toxic proteins and damaged organelles, thereby promoting cellular health and preventing the accumulation of cellular debris that can contribute to aging and disease. Fasting essentially acts as a "reset" button, enhancing the efficiency of this process.
- Removes damaged mitochondria: These powerhouses of the cell can become dysfunctional over time, contributing to cellular dysfunction. Autophagy removes them, replacing them with healthier mitochondria.
- Recycles cellular components: Provides building blocks for new cell components, thus conserving resources during fasting.
- Reduces cellular stress: By removing damaged components, autophagy reduces overall stress on the cell, leading to improved function.
Changes in Gene Expression
Fasting alters the expression of numerous genes, impacting cellular processes related to metabolism, stress response, and inflammation. Specific genes involved in protecting cells against oxidative stress and promoting longevity are often upregulated during fasting periods. Conversely, genes associated with inflammation and disease risk may be downregulated. The precise changes are dependent on the duration and type of fast, and ongoing research aims to further elucidate these complex transcriptional alterations.
- Increased expression of stress-resistance genes: Helping cells better withstand various forms of cellular stress.
- Decreased expression of inflammatory genes: Reducing chronic inflammation, which is implicated in numerous diseases.
- Altered metabolic gene expression: Shifting the cell's metabolism towards utilizing fat stores for energy.
Metabolic Switching
During fasting, cells undergo a metabolic switch, transitioning from primarily using glucose (sugar) as fuel to utilizing stored fat. This process, known as ketogenesis, leads to the production of ketone bodies, which serve as an alternative energy source for many cells. Ketones offer a more efficient and sustained energy supply compared to glucose, improving cellular function and potentially reducing the risk of oxidative stress. The extent of this metabolic switch depends on the duration and type of fast.
- Increased ketone body production: Providing an alternative fuel source for the cells.
- Reduced reliance on glucose: Conserving glucose stores and promoting fat utilization.
- Improved mitochondrial function: Ketones can improve mitochondrial efficiency and reduce oxidative stress.
Cellular Repair and Regeneration
The cellular cleanup associated with autophagy, coupled with the reduction in inflammation and improved metabolic efficiency, creates an environment conducive to cellular repair and regeneration. Fasting can stimulate the production of new cells in certain tissues and enhance the repair of damaged ones. This is particularly relevant in contexts such as wound healing and tissue regeneration.
- Enhanced stem cell activity: Stimulating the production of new cells to replace damaged ones.
- Improved tissue repair: Accelerating the healing process in damaged tissues.
- Reduced inflammation: Creating a more favorable environment for tissue repair.
Hormonal Changes Affecting Cells
Fasting triggers significant hormonal changes throughout the body, and these hormonal shifts directly impact cellular processes. Levels of hormones like insulin decrease, while levels of hormones like glucagon and growth hormone increase. These alterations affect nutrient sensing pathways within cells, influencing various cellular processes including metabolism, protein synthesis, and cellular growth. The hormonal changes also contribute to the upregulation of autophagy and other beneficial cellular processes.
- Insulin reduction: Decreased insulin signaling reduces glucose uptake and promotes fat utilization.
- Glucagon increase: Promotes the breakdown of glycogen (stored glucose) and the production of glucose from other sources.
- Growth hormone increase: Supports cellular repair and regeneration processes.
Does fasting actually repair damaged cells?
While fasting doesn't directly "repair" damaged cells in the way a surgeon fixes a broken bone, there's growing evidence it can significantly influence cellular processes that promote healing and regeneration. The mechanisms aren't fully understood, but research suggests several pathways. Autophagy, a process where cells break down and recycle damaged components, is significantly boosted during fasting. This cellular "clean-up crew" removes dysfunctional proteins and organelles, improving cellular health and function. Furthermore, fasting can reduce inflammation, a major contributor to cellular damage in many diseases. Chronic inflammation damages cells and tissues, and fasting can help mitigate this by reducing inflammatory markers. However, it's crucial to note that fasting isn't a magic bullet. Severe or irreversible cell damage may not be reversed by fasting alone. Its benefits are most pronounced when combined with other healthy lifestyle choices like regular exercise and a balanced diet. The extent of cellular repair depends on various factors, including the type and extent of damage, the individual's overall health, and the fasting protocol employed. More research is needed to fully elucidate the impact of fasting on different cell types and disease states, but the preliminary findings are encouraging regarding its potential role in cellular maintenance and regeneration.
What types of cells are most affected by fasting?
The effects of fasting on cells aren't uniform across all cell types. While research is still ongoing, some cell types seem more responsive than others. Studies suggest that fasting particularly impacts cells with high metabolic rates or those prone to damage from oxidative stress. For example, immune cells exhibit significant changes during fasting, with some studies showing an improvement in immune function and a reduction in inflammatory responses. Furthermore, cells in certain organs, such as the liver and brain, show adaptive changes in response to fasting, promoting cellular resilience and enhancing their ability to withstand stress. Cancer cells have also been shown to be vulnerable to fasting, with some research suggesting that fasting can inhibit their growth and proliferation. However, this is a complex area and requires further investigation. The precise cellular mechanisms and the specific cell types most affected by fasting remain areas of active investigation, and the impact may vary depending on factors like the duration and type of fasting, individual health status, and the specific cell type in question.
Can fasting reverse aging at a cellular level?
The idea of fasting reversing aging at a cellular level is a fascinating and complex one. While there's considerable excitement surrounding the potential anti-aging benefits of fasting, it's essential to approach this with nuance. Fasting can influence several cellular processes associated with aging. It can activate autophagy, which helps remove damaged cells and cellular debris, a hallmark of aging. Moreover, fasting can reduce oxidative stress, a major contributor to aging. However, it's crucial to understand that fasting is unlikely to completely "reverse" aging. It's more accurate to say that fasting may slow down some aspects of cellular aging and potentially extend healthspan, which is the period of life spent in good health, rather than lifespan. The concept of reversing aging completely remains a significant challenge in science, and while fasting offers promising avenues for improving cellular health, it's not a guaranteed anti-aging elixir. More research is needed to fully understand the long-term effects of fasting on various markers of aging.
Are there any risks associated with fasting and cellular health?
While fasting can offer potential benefits for cellular health, it's not without potential risks, especially if not done correctly. Improper fasting can lead to several adverse effects. Nutrient deficiencies can arise if fasting is prolonged or not planned carefully, potentially leading to cellular dysfunction. Furthermore, some individuals may experience negative side effects such as headaches, dizziness, fatigue, and irritability, especially in the initial stages of fasting. Individuals with certain medical conditions, such as diabetes, eating disorders, or pregnant or breastfeeding women, should consult with their physician before embarking on any fasting regimen. Moreover, the type and duration of fasting are crucial considerations. Extreme or prolonged fasting can be harmful and should be undertaken only under medical supervision. It's also important to reintroduce food gradually after fasting to avoid any digestive issues. In summary, while fasting can positively impact cellular health for many, it's vital to approach it responsibly and consider potential risks. Proper planning, medical guidance where necessary, and a gradual approach are key to maximizing benefits and minimizing risks.
Deja una respuesta