What are the four types of mouth sores
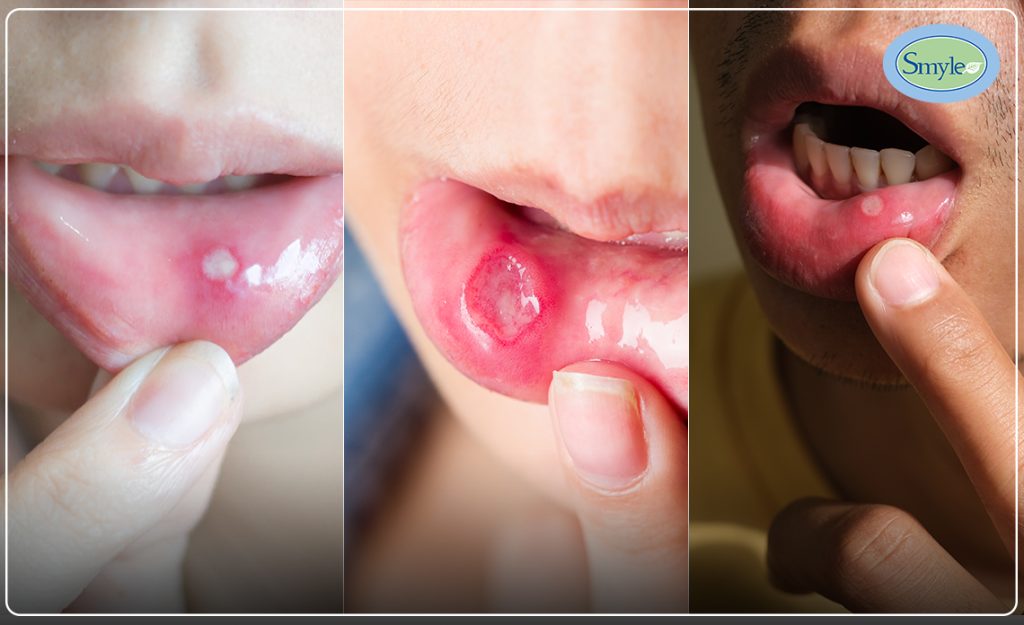
Mouth sores, also known as canker sores or aphthous ulcers, are a common ailment that can affect people of all ages. They can be painful and uncomfortable, and they often interfere with eating, drinking, and talking. There are four main types of mouth sores, each with its own unique characteristics and causes. In this article, we will discuss the four types of mouth sores and provide tips for preventing and treating them.
What are the Four Main Types of Mouth Sores?
While many different types of sores can appear in the mouth, four main categories encompass most common occurrences. These categories are based on the underlying cause and appearance of the sore. It's important to note that if you're experiencing persistent or unusual mouth sores, you should consult a dentist or doctor for proper diagnosis and treatment.
Aphthous Ulcers (Canker Sores)
Aphthous ulcers, commonly known as canker sores, are small, shallow lesions that usually appear on the tongue, inner cheeks, or lips. They are typically round or oval in shape and have a white or yellowish base surrounded by a red border. They are not contagious and usually heal within 1-3 weeks without scarring. The exact cause is unknown, but factors like stress, trauma, hormonal changes, and nutritional deficiencies have been linked to their development. Symptoms may include mild to moderate pain, burning, or tingling sensation before the sore appears.
Cold Sores (Fever Blisters)
Cold sores, or fever blisters, are caused by the herpes simplex virus (HSV). These sores typically appear on the lips and surrounding skin, unlike canker sores which are usually inside the mouth. They start as a tingling or burning sensation, followed by the development of small, fluid-filled blisters that eventually crust over. Cold sores are highly contagious and can spread through direct contact. Outbreaks can be triggered by stress, sun exposure, illness, or hormonal changes. Treatment often involves antiviral medications to shorten the duration and severity of the outbreak.
Herpetic Gingivostomatitis
Herpetic gingivostomatitis is a more severe form of oral herpes infection. It typically occurs in young children and is characterized by widespread sores throughout the mouth, including the gums (gingiva), tongue, and inner cheeks. These sores can be painful and can make eating and drinking difficult. Fever, swollen lymph nodes, and general malaise (a feeling of illness) are also common symptoms. This condition requires medical attention and is usually treated with antiviral medication. This is caused by the same virus that causes cold sores (HSV).
Traumatic Ulcers
Traumatic ulcers are caused by injury or irritation to the mouth's lining. This can be from biting your cheek, accidentally scraping your mouth with a toothbrush, or from ill-fitting dentures. These sores are usually shallow and heal quickly once the irritating factor is removed. They are typically not painful unless significantly large or infected. Treatment usually involves removing the irritant and practicing good oral hygiene.
Types of Mouth Sores Summary
| Type of Mouth Sore | Cause | Location | Symptoms | Contagious |
|---|---|---|---|---|
| Aphthous Ulcers (Canker Sores) | Unknown, but possibly stress, trauma, hormonal changes | Tongue, inner cheeks, lips (inside the mouth) | Pain, burning, white/yellow base with red border | No |
| Cold Sores (Fever Blisters) | Herpes simplex virus (HSV) | Lips and surrounding skin | Tingling, burning, fluid-filled blisters, crusting | Yes |
| Herpetic Gingivostomatitis | Herpes simplex virus (HSV) | Gums, tongue, inner cheeks (widespread) | Numerous painful sores, fever, swollen lymph nodes | Yes |
| Traumatic Ulcers | Injury or irritation | Anywhere in the mouth | Shallow sore, may or may not be painful | No |
What are the Four Main Types of Mouth Sores?
While many different types of sores can appear in the mouth, four main categories encompass most common occurrences. These categories are based on the underlying cause and appearance of the sore. It's important to note that if you're experiencing persistent or unusual mouth sores, you should consult a dentist or doctor for proper diagnosis and treatment.
Aphthous Ulcers (Canker Sores)
Aphthous ulcers, commonly known as canker sores, are small, shallow lesions that usually appear on the tongue, inner cheeks, or lips. They are typically round or oval in shape and have a white or yellowish base surrounded by a red border. They are not contagious and usually heal within 1-3 weeks without scarring. The exact cause is unknown, but factors like stress, trauma, hormonal changes, and nutritional deficiencies have been linked to their development. Symptoms may include mild to moderate pain, burning, or tingling sensation before the sore appears.
Cold Sores (Fever Blisters)
Cold sores, or fever blisters, are caused by the herpes simplex virus (HSV). These sores typically appear on the lips and surrounding skin, unlike canker sores which are usually inside the mouth. They start as a tingling or burning sensation, followed by the development of small, fluid-filled blisters that eventually crust over. Cold sores are highly contagious and can spread through direct contact. Outbreaks can be triggered by stress, sun exposure, illness, or hormonal changes. Treatment often involves antiviral medications to shorten the duration and severity of the outbreak.
Herpetic Gingivostomatitis
Herpetic gingivostomatitis is a more severe form of oral herpes infection. It typically occurs in young children and is characterized by widespread sores throughout the mouth, including the gums (gingiva), tongue, and inner cheeks. These sores can be painful and can make eating and drinking difficult. Fever, swollen lymph nodes, and general malaise (a feeling of illness) are also common symptoms. This condition requires medical attention and is usually treated with antiviral medication. This is caused by the same virus that causes cold sores (HSV).
Traumatic Ulcers
Traumatic ulcers are caused by injury or irritation to the mouth's lining. This can be from biting your cheek, accidentally scraping your mouth with a toothbrush, or from ill-fitting dentures. These sores are usually shallow and heal quickly once the irritating factor is removed. They are typically not painful unless significantly large or infected. Treatment usually involves removing the irritant and practicing good oral hygiene.
Types of Mouth Sores Summary
| Type of Mouth Sore | Cause | Location | Symptoms | Contagious |
|---|---|---|---|---|
| Aphthous Ulcers (Canker Sores) | Unknown, but possibly stress, trauma, hormonal changes | Tongue, inner cheeks, lips (inside the mouth) | Pain, burning, white/yellow base with red border | No |
| Cold Sores (Fever Blisters) | Herpes simplex virus (HSV) | Lips and surrounding skin | Tingling, burning, fluid-filled blisters, crusting | Yes |
| Herpetic Gingivostomatitis | Herpes simplex virus (HSV) | Gums, tongue, inner cheeks (widespread) | Numerous painful sores, fever, swollen lymph nodes | Yes |
| Traumatic Ulcers | Injury or irritation | Anywhere in the mouth | Shallow sore, may or may not be painful | No |
What do autoimmune mouth sores look like?

Autoimmune mouth sores, often associated with conditions like Behçet's disease, lupus, or Crohn's disease, can vary significantly in appearance depending on the underlying condition and its severity. They aren't always easily distinguishable from other types of mouth sores. However, some common characteristics include:
Painful ulcers: These are usually the most prominent symptom. The pain can range from mild discomfort to severe, making eating and speaking difficult.
Size and shape: They can be small and superficial, or large and deep, with irregular borders. Unlike canker sores, which are usually round or oval, autoimmune mouth sores can be more irregularly shaped.
Location: They can appear anywhere in the mouth, including the tongue, lips, cheeks, gums, and palate.
Color: They typically present as reddish or purplish lesions, often with a yellowish or grayish-white base. They may also be surrounded by a reddish halo.
Duration: They can persist for days or weeks, and often recur. The frequency and duration of recurrence can vary depending on the autoimmune condition.
Appearance of Mouth Sores in Behçet's Disease
Behçet's disease is a systemic vasculitis that can manifest as recurrent oral ulcers. These ulcers are typically painful and deep, often appearing as multiple, shallow lesions. They are usually surrounded by a reddish halo and can take a significant amount of time to heal. The recurrent nature of these lesions is a hallmark of the disease.
- Multiple lesions: Several sores are frequently present simultaneously.
- Rapid healing and recurrence: While sores eventually heal, they tend to reappear frequently.
- Deep ulcers: Unlike some other mouth sores, these ulcers often penetrate deeper into the mucous membranes.
Mouth Sores Associated with Lupus
Lupus is an autoimmune disease affecting multiple organ systems. Oral manifestations can include ulcers, which may appear as painful sores with a reddish or purplish hue. They are often accompanied by other lupus symptoms like fatigue, joint pain, and skin rashes. The appearance of these ulcers can be quite variable, and they may be less severe than those seen in Behçet's.
- Variety in appearance: The size, shape, and severity of sores vary greatly between individuals and even within the same individual over time.
- Association with other symptoms: Oral ulcers are frequently accompanied by other symptoms of lupus.
- Pain level varies: The degree of pain experienced can differ significantly from person to person.
Oral Manifestations of Crohn's Disease
Crohn's disease, an inflammatory bowel disease, can sometimes manifest with oral lesions. These often appear as aphthous-like ulcers, which are small, shallow sores. They can be painful and may be located anywhere in the mouth. These are usually not as severe as those associated with Behçet's or systemic lupus erythematosus.
- Smaller, shallower ulcers: Often less deep and extensive than in Behçet’s.
- Similar to aphthous ulcers: The appearance often resembles common canker sores but may occur in greater numbers.
- Correlation with disease activity: The presence and severity of oral ulcers may correlate with the overall activity of Crohn's disease.
Differentiating Autoimmune Mouth Sores from Other Types of Mouth Sores
It's crucial to differentiate autoimmune mouth sores from other types of oral ulcers, such as canker sores or herpes simplex lesions. Autoimmune sores may be more persistent, painful, and numerous than other types of mouth sores. Their irregular shape and color can also be distinguishing features. A proper diagnosis from a medical professional is essential for appropriate treatment.
- Persistence and Recurrence: Autoimmune sores tend to recur frequently and persist for longer periods.
- Pain Level: They are often more painful than canker sores.
- Number and Distribution: Typically, multiple sores are present across the mouth.
Seeking Medical Attention for Mouth Sores
If you experience recurrent, painful mouth sores, especially those with unusual characteristics, it's important to seek medical advice. A healthcare professional can properly diagnose the underlying cause, whether it's an autoimmune condition or something else, and provide appropriate treatment to manage your symptoms and improve your oral health. Early diagnosis and treatment are crucial for managing autoimmune conditions.
- Prompt medical consultation: Do not delay seeking professional help if you suspect an autoimmune related oral ulcer.
- Accurate diagnosis: A doctor can distinguish between different types of mouth sores and determine the underlying cause.
- Effective treatment: Treatment plans can vary based on the underlying condition and its severity.
When should you worry about mouth sores?

When Should You Worry About Mouth Sores?
Mouth sores, also known as aphthous ulcers or canker sores, are common and usually heal on their own within a week or two. However, there are instances when you should seek medical attention. Persistent sores that don't heal, unusually large or painful sores, sores accompanied by other symptoms, and sores that occur frequently are all reasons to consult a doctor or dentist. Ignoring potentially serious underlying conditions can lead to complications, so it's crucial to be aware of when a simple mouth sore warrants professional evaluation.
Persistent Sores
A mouth sore that lasts longer than two weeks without showing signs of healing should be checked by a healthcare professional. This prolonged duration could indicate an underlying issue, such as an infection, vitamin deficiency, or even a more serious condition. Delaying treatment can lead to secondary infections or complications.
- Prolonged healing time: More than 2 weeks without improvement.
- Increasing size or depth: The sore is getting larger or deeper over time.
- Lack of response to home remedies: Over-the-counter treatments are ineffective.
Unusually Large or Painful Sores
While typical canker sores are small and relatively manageable, abnormally large or intensely painful sores could signal a problem. These sores might be indicative of a more serious condition requiring specific treatment. It's important to note that pain levels can vary significantly, and severe pain warrants immediate attention.
- Size: Sores significantly larger than typical canker sores (greater than 1 cm in diameter).
- Depth: Deep ulcers that extend beyond the surface layers of the mouth.
- Pain level: Intense pain that interferes with eating, drinking, or speaking.
Mouth Sores Accompanied by Other Symptoms
The presence of mouth sores alongside other symptoms is a strong indicator that something more serious is at play. Fever, fatigue, swollen lymph nodes, skin rashes, or joint pain, in combination with mouth sores, require immediate medical evaluation. These symptoms may indicate an underlying infection or autoimmune disease.
- Fever: High body temperature (above 100.4°F or 38°C).
- Fatigue: Unusual tiredness or weakness.
- Swollen lymph nodes: Swollen glands in the neck, jaw, or armpits.
Frequent Occurrences of Mouth Sores
If you experience mouth sores frequently, perhaps several times a month, you should seek professional advice. Recurring sores, even if seemingly minor, can suggest a hidden medical issue that needs to be addressed. The frequency of sores is a significant factor in determining the necessity for medical evaluation.
- Frequency: Multiple occurrences of mouth sores within a short period (e.g., several times per month).
- Pattern: Noticeable pattern to the occurrences (e.g., always after certain foods or stress).
- Severity: Even if individual sores are minor, frequent occurrences indicate a potential problem.
Sores That Don't Respond to Treatment
Mouth sores that persist despite using home remedies or over-the-counter treatments should be evaluated by a doctor or dentist. Failure to respond to treatment might suggest a more complex underlying cause that requires specific medical intervention. Do not assume the sore will eventually heal on its own; consult a healthcare provider for proper diagnosis and treatment.
- Lack of improvement: No visible healing after several days or weeks of self-treatment.
- Worsening symptoms: The sores are getting larger, more painful, or more numerous despite treatment.
- New symptoms: The development of additional symptoms (e.g., fever, fatigue) while using treatment.
What heals mouth sores the fastest?
What Heals Mouth Sores the Fastest?
There's no single magic cure for mouth sores (also known as aphthous ulcers or canker sores), as healing time varies depending on their size, cause, and individual factors. However, several approaches can significantly speed up the healing process. Generally, smaller sores heal faster than larger ones, and most heal within 1-3 weeks without intervention. However, using the right treatments can shorten that timeline considerably. It's also crucial to identify the underlying cause, as addressing that can be key to prevention and faster healing.
1. Over-the-Counter Medications
Many over-the-counter (OTC) medications can ease pain and promote faster healing of mouth sores. These often contain anesthetic agents to numb the area and reduce discomfort, and sometimes include ingredients that accelerate healing.
- Oral analgesics: These medications, like benzocaine or lidocaine, can be applied topically to numb the affected area, providing relief from pain.
- Antiseptic mouthwashes: These can help to clean the mouth, reduce bacterial load and prevent infection, which could prolong healing. Look for mouthwashes containing ingredients like chlorhexidine or hydrogen peroxide.
- Topical corticosteroids: These are available in gel or ointment form and can reduce inflammation and pain, leading to faster healing. However, prolonged use is generally discouraged, and only recommended under the direction of a dentist or doctor.
2. Home Remedies
Several home remedies can provide relief and potentially speed up healing. These are often gentler than OTC medications and can be easily implemented at home. It's important to remember that results vary widely, and these are not replacements for professional medical advice.
- Saltwater rinses: Rinsing your mouth with warm salt water several times a day can help to clean the sore and reduce inflammation. The salt acts as a natural antiseptic.
- Ice: Applying ice to the affected area can help to numb the pain and reduce swelling. Wrap the ice in a cloth to avoid direct contact with the skin.
- Aloe vera: Applying aloe vera gel directly to the sore can soothe the area and promote healing. It is a natural anti-inflammatory and contains compounds known to accelerate tissue regeneration.
3. Maintaining Good Oral Hygiene
Excellent oral hygiene is crucial for preventing mouth sores and promoting faster healing if they do occur. Poor hygiene can increase the risk of infection and prolong the healing time.
- Regular brushing and flossing: Gentle brushing and flossing help remove food particles and plaque that can irritate the sores and delay healing.
- Avoid irritating foods: Spicy, acidic, or hard foods can further irritate the sore and slow down the healing process. Consider a soft food diet until it heals.
- Stay hydrated: Drinking plenty of water keeps the mouth moist and helps to prevent further irritation.
4. Addressing Underlying Medical Conditions
Sometimes, mouth sores are a symptom of an underlying medical condition, like vitamin deficiencies (particularly B12 and iron), autoimmune diseases, or certain medications. Treating the underlying cause is critical for preventing recurrence and speeding up healing. A visit to a healthcare professional is necessary for diagnosis.
- Dietary changes: If a deficiency is identified, a change in diet or supplementation is often helpful.
- Medical treatment: Addressing the underlying medical condition directly might require medication or other treatments.
- Medication review: If certain medications are contributing to the mouth sores, your doctor may recommend an alternative.
5. When to See a Doctor
While most mouth sores heal on their own, it's important to seek medical attention if you experience any of the following: sores that are unusually large, persistent, or painful; sores that bleed excessively; a fever; difficulty swallowing or breathing; or if you have sores accompanied by other symptoms such as swollen lymph nodes. These could indicate a more serious underlying health issue that needs prompt evaluation and treatment.
- Persistent sores: Sores that don't heal within 2-3 weeks warrant a medical check-up.
- Severe pain: Intense pain that interferes with eating or drinking may require medical intervention.
- Recurring sores: Frequent outbreaks of mouth sores might point towards a deeper issue requiring medical management.
What health issues cause mouth sores?
What Health Issues Cause Mouth Sores?
Mouth sores, also known as oral ulcers or aphthous ulcers, can be caused by a variety of factors. They are generally characterized by small, shallow lesions that develop on the soft tissues in the mouth, including the tongue, cheeks, lips, and gums. The causes can range from minor irritations to underlying medical conditions. While many mouth sores heal on their own within a week or two, persistent or recurring sores warrant a visit to a doctor or dentist to rule out more serious issues.
Viral Infections
Several viruses can trigger the development of mouth sores. Herpes simplex virus (HSV), responsible for cold sores, is a common culprit. These sores typically appear on the lips and surrounding skin. Other viral infections like hand, foot, and mouth disease, chickenpox, and even the common cold can sometimes manifest as oral ulcers. The sores related to these viral infections often exhibit distinct characteristics that help in diagnosis.
- HSV-1: Often presents as cold sores, typically clustered blisters that crust over.
- Hand, foot, and mouth disease: Characterized by small, painful blisters in the mouth, hands, and feet.
- Chickenpox: Causes small, fluid-filled blisters throughout the body, including the mouth.
Bacterial Infections
While less common than viral infections, bacterial infections can also lead to mouth sores. Poor oral hygiene can create an environment conducive to bacterial overgrowth, resulting in sores. Specific bacterial infections, like strep throat (streptococcal pharyngitis), can sometimes have oral manifestations. Aggressive treatment of bacterial infections is vital to prevent complications.
- Poor oral hygiene: Neglecting brushing and flossing allows bacteria to thrive, leading to gum disease and mouth sores.
- Infectious mononucleosis ("mono"): Can cause mouth ulcers as one of its symptoms.
- Untreated dental infections: Infections in teeth or gums can spread, causing ulcers.
Nutritional Deficiencies
Deficiencies in certain vitamins and minerals, such as vitamin B12, iron, and folic acid, can increase the susceptibility to mouth sores. These deficiencies can weaken the immune system and make individuals more prone to developing ulcers. A balanced diet rich in these nutrients is crucial for maintaining oral health.
- Vitamin B12 deficiency: Can cause glossitis (inflammation of the tongue) and mouth sores.
- Iron deficiency anemia: Can lead to fatigue, pale skin, and mouth sores.
- Folic acid deficiency: Can affect cell growth and increase the risk of mouth sores.
Autoimmune Diseases
Several autoimmune diseases, where the body's immune system attacks its own tissues, can cause mouth sores as a symptom. Behçet's disease and inflammatory bowel disease (IBD) are examples of conditions that frequently present with oral ulcers. These conditions often require specialized medical attention for effective management.
- Behçet's disease: A chronic inflammatory condition characterized by recurrent mouth sores, genital ulcers, and eye inflammation.
- Inflammatory bowel disease (IBD): Including Crohn's disease and ulcerative colitis, can cause mouth sores as a manifestation.
- Systemic lupus erythematosus (SLE): An autoimmune disease that can affect multiple organs, including the mouth.
Allergies and Irritants
Certain foods, dental products, and even medications can trigger allergic reactions or irritation that lead to mouth sores. Food allergies, particularly to citrus fruits, nuts, or certain spices, are common culprits. Dental appliances like braces or dentures can also cause sores due to friction or pressure. Identifying and avoiding these triggers is key to preventing recurring sores.
- Allergic reactions: To foods, medications, or dental products.
- Irritants: Such as acidic foods, hot beverages, or certain mouthwashes.
- Trauma: Accidental biting, burns, or injuries to the mouth.
What are the four main types of mouth sores?
While there isn't a universally agreed-upon classification of "four main types" of mouth sores, we can categorize them into four common and distinct presentations based on their cause and appearance. These are: aphthous ulcers (canker sores), cold sores (fever blisters), herpetic gingivostomatitis, and mouth sores caused by trauma or injury. It's crucial to understand that other conditions can also manifest as mouth sores, such as fungal infections (oral thrush), bacterial infections, or certain systemic diseases. However, these four categories encompass a large percentage of common mouth sore experiences. Aphthous ulcers are small, shallow lesions that typically appear on the inner cheeks, lips, or tongue. They are usually painful but resolve on their own within a week or two. Cold sores, caused by the herpes simplex virus (HSV-1), are characterized by fluid-filled blisters that often appear on the lips and surrounding skin. These blisters typically crust over and heal within a week to ten days. Herpetic gingivostomatitis is a more severe form of oral herpes infection, often occurring in young children, causing widespread blisters and ulcers in the mouth and gums. It typically requires medical attention. Finally, mouth sores from trauma can result from accidental biting, burns, or irritation from sharp tooth edges or ill-fitting dentures. These sores typically heal quickly once the underlying cause is addressed.
What causes canker sores (aphthous ulcers)?
The exact cause of aphthous ulcers, or canker sores, remains unknown, but several factors are thought to contribute to their development. Stress is a commonly cited trigger, with many individuals experiencing outbreaks during periods of high anxiety or pressure. Minor injuries to the mouth's lining, such as biting the cheek or accidentally scraping the tongue, can also initiate the formation of these sores. Certain foods, particularly acidic or spicy ones, can irritate the mouth and potentially exacerbate existing canker sores or trigger new ones. Hormonal changes, particularly those experienced during menstruation, can also play a role in the onset of aphthous ulcers. Nutritional deficiencies, especially a lack of certain vitamins and minerals like iron, B vitamins (such as B12 and folate), and zinc, are also linked to an increased likelihood of developing canker sores. Finally, some autoimmune conditions and allergic reactions have been associated with canker sore development. It's important to note that for many people, the precise trigger remains elusive, and outbreaks may occur sporadically without an identifiable cause. While these factors are often implicated, further research is needed to fully understand the complex interplay leading to aphthous ulcer formation.
How can I tell the difference between a canker sore and a cold sore?
Differentiating between canker sores (aphthous ulcers) and cold sores (fever blisters) is crucial for appropriate treatment and understanding the underlying cause. Canker sores typically appear inside the mouth, on the cheeks, gums, tongue, or soft palate. They are usually round or oval, have a yellowish or whitish base, and are surrounded by a red halo. They are often painful and can last for a week or two. Importantly, canker sores are not contagious. Cold sores, on the other hand, are caused by the herpes simplex virus (HSV-1) and appear on the outer lips, around the mouth, and rarely inside the mouth. They begin as small blisters that quickly become fluid-filled before crusting over. Unlike canker sores, cold sores are contagious and can be spread through direct contact. The pain associated with cold sores can vary but is generally less intense than the pain of canker sores. While both can be uncomfortable, their location, appearance, and infectious nature are key distinguishing features. If you are unsure, consulting a doctor or dentist for a proper diagnosis is always recommended.
When should I see a doctor about mouth sores?
While many mouth sores resolve on their own, there are certain situations where seeking medical attention is crucial. If a mouth sore is unusually large, deep, or persistent (lasting longer than two weeks), it's important to consult a doctor or dentist. Similarly, if you experience multiple sores simultaneously, or if they are accompanied by fever, swollen lymph nodes, or difficulty swallowing, immediate medical attention is warranted. Mouth sores that bleed excessively or don't heal despite home remedies should also be evaluated by a healthcare professional. Furthermore, if you suspect a mouth sore may be caused by an infection, such as oral thrush (candidiasis) or herpes gingivostomatitis, it's essential to seek appropriate treatment to prevent complications. Individuals with weakened immune systems should also seek medical advice for any mouth sores, as they may be more susceptible to severe infections. Lastly, if you have recurring mouth sores that significantly impact your quality of life, consulting a doctor can help identify potential underlying causes and explore treatment options to prevent future outbreaks. Early diagnosis and treatment can often prevent complications and ensure a faster recovery.
Deja una respuesta