What is a sore tongue a symptom of
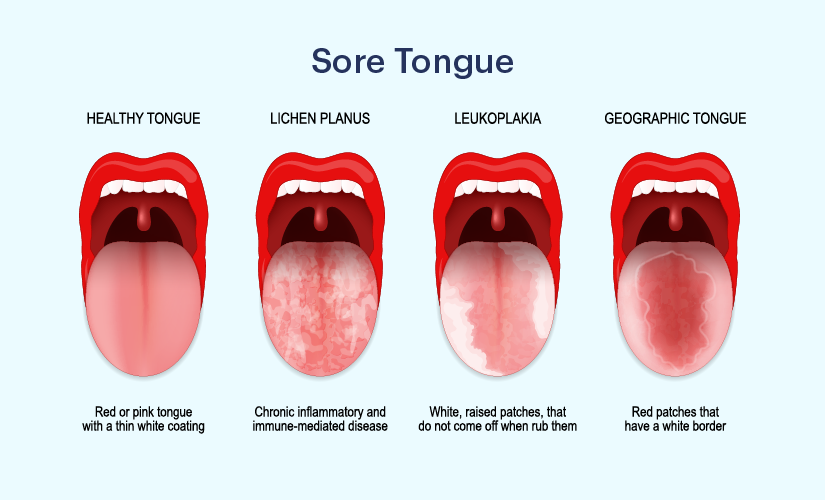
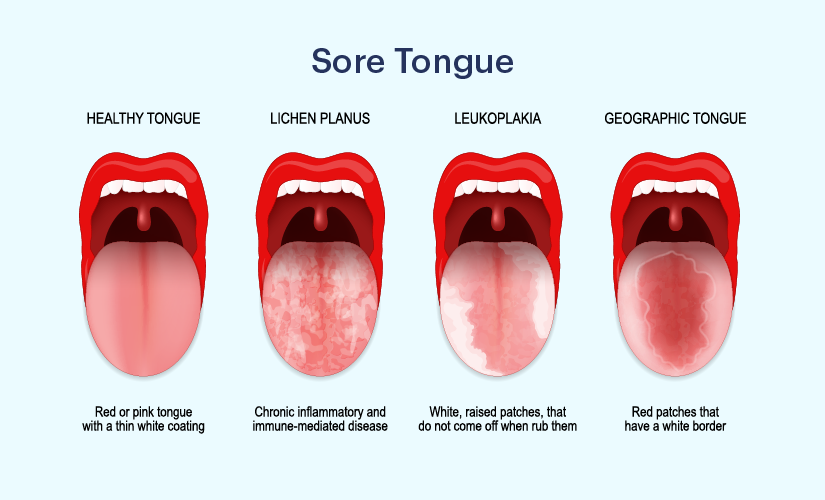
A sore tongue, also known as glossitis, is a common condition that can cause discomfort and interfere with speaking, eating, and drinking. While it is often a minor inconvenience, a sore tongue can also be a sign of an underlying medical condition.
Understanding the causes of a sore tongue can help you determine the best course of treatment. This article will explore the various medical conditions that can cause a sore tongue and provide guidance on when to seek professional help.
What is a Sore Tongue a Symptom Of?
A sore tongue, medically known as glossitis, can be a symptom of a wide range of conditions, from minor irritations to more serious underlying health issues. The cause of the soreness is crucial in determining the appropriate treatment. A simple sore tongue might resolve on its own with some home remedies, while a persistent or severe sore tongue requires a visit to a doctor or dentist for proper diagnosis and management. The appearance of the tongue – its color, texture, and the presence of any lesions – can provide valuable clues to the underlying cause.
Nutritional Deficiencies
A sore tongue can be a sign of vitamin deficiencies, particularly deficiencies in B vitamins like B12, riboflavin (B2), niacin (B3), and folate (B9). These vitamins are essential for maintaining the health of the oral mucosa, and their deficiency can lead to inflammation and soreness of the tongue. Iron deficiency can also manifest as a sore tongue. Symptoms often include a smooth, pale, or red tongue. A blood test can help determine if nutritional deficiencies are the cause.
Infections
Various infections can cause a sore tongue. Oral thrush, a fungal infection caused by Candida albicans, is a common culprit, presenting as white patches or a creamy coating on the tongue. Bacterial infections can also lead to soreness and inflammation. Viral infections, such as those causing the common cold or flu, can sometimes lead to a secondary sore tongue due to dehydration and reduced saliva production. Antibiotics or antifungals may be necessary for treatment, depending on the type of infection.
Allergies
Food allergies or sensitivities can trigger an inflammatory response in the mouth and tongue, resulting in soreness, swelling, and even blisters. Certain medications or mouthwashes can also cause allergic reactions, leading to similar symptoms. Identifying and avoiding the allergen is key in managing this condition. In severe cases, an antihistamine may be necessary.
Mouth Injuries and Irritation
Physical trauma to the tongue, such as biting it accidentally or experiencing a burn from hot food or drinks, can cause obvious soreness and inflammation. Irritants like strong mouthwashes, certain foods, or even smoking can also irritate the tongue, leading to discomfort. Treatment usually involves avoiding the irritant and allowing the injury to heal naturally. For burns, applying a cold compress can provide relief.
Underlying Medical Conditions
In some cases, a sore tongue can be a symptom of a more serious underlying medical condition. Geographic tongue, a benign condition characterized by patches of smooth, red areas on the tongue, is one example. Other conditions like Behçet's disease, Kawasaki disease, and certain autoimmune diseases can also manifest with a sore tongue as one of their symptoms. Prompt medical attention is necessary to diagnose and treat these conditions.
| Symptom | Possible Causes | Treatment |
|---|---|---|
| Sore, red tongue | Vitamin deficiencies, infections, allergies | Dietary changes, medication (antibiotics, antifungals, antihistamines) |
| White patches on tongue | Oral thrush | Antifungal medication |
| Burning sensation | Geographic tongue, nutritional deficiencies, irritation | Avoid irritants, dietary changes, medication (depending on the cause) |
| Swollen tongue | Allergies, infections, injury | Antihistamines, antibiotics, wound care |
| Smooth, pale tongue | Iron deficiency, pernicious anemia | Iron supplements, vitamin B12 injections |
What is a Sore Tongue a Symptom Of?
A sore tongue, medically known as glossitis, can be a symptom of a wide range of conditions, from minor irritations to more serious underlying health issues. The cause of the soreness is crucial in determining the appropriate treatment. A simple sore tongue might resolve on its own with some home remedies, while a persistent or severe sore tongue requires a visit to a doctor or dentist for proper diagnosis and management. The appearance of the tongue – its color, texture, and the presence of any lesions – can provide valuable clues to the underlying cause.
Nutritional Deficiencies
A sore tongue can be a sign of vitamin deficiencies, particularly deficiencies in B vitamins like B12, riboflavin (B2), niacin (B3), and folate (B9). These vitamins are essential for maintaining the health of the oral mucosa, and their deficiency can lead to inflammation and soreness of the tongue. Iron deficiency can also manifest as a sore tongue. Symptoms often include a smooth, pale, or red tongue. A blood test can help determine if nutritional deficiencies are the cause.
Infections
Various infections can cause a sore tongue. Oral thrush, a fungal infection caused by Candida albicans, is a common culprit, presenting as white patches or a creamy coating on the tongue. Bacterial infections can also lead to soreness and inflammation. Viral infections, such as those causing the common cold or flu, can sometimes lead to a secondary sore tongue due to dehydration and reduced saliva production. Antibiotics or antifungals may be necessary for treatment, depending on the type of infection.
Allergies
Food allergies or sensitivities can trigger an inflammatory response in the mouth and tongue, resulting in soreness, swelling, and even blisters. Certain medications or mouthwashes can also cause allergic reactions, leading to similar symptoms. Identifying and avoiding the allergen is key in managing this condition. In severe cases, an antihistamine may be necessary.
Mouth Injuries and Irritation
Physical trauma to the tongue, such as biting it accidentally or experiencing a burn from hot food or drinks, can cause obvious soreness and inflammation. Irritants like strong mouthwashes, certain foods, or even smoking can also irritate the tongue, leading to discomfort. Treatment usually involves avoiding the irritant and allowing the injury to heal naturally. For burns, applying a cold compress can provide relief.
Underlying Medical Conditions
In some cases, a sore tongue can be a symptom of a more serious underlying medical condition. Geographic tongue, a benign condition characterized by patches of smooth, red areas on the tongue, is one example. Other conditions like Behçet's disease, Kawasaki disease, and certain autoimmune diseases can also manifest with a sore tongue as one of their symptoms. Prompt medical attention is necessary to diagnose and treat these conditions.
| Symptom | Possible Causes | Treatment |
|---|---|---|
| Sore, red tongue | Vitamin deficiencies, infections, allergies | Dietary changes, medication (antibiotics, antifungals, antihistamines) |
| White patches on tongue | Oral thrush | Antifungal medication |
| Burning sensation | Geographic tongue, nutritional deficiencies, irritation | Avoid irritants, dietary changes, medication (depending on the cause) |
| Swollen tongue | Allergies, infections, injury | Antihistamines, antibiotics, wound care |
| Smooth, pale tongue | Iron deficiency, pernicious anemia | Iron supplements, vitamin B12 injections |
What is the most common cause of a sore tongue?
The most common cause of a sore tongue is aphthous ulcers, also known as canker sores. These are small, shallow ulcers that develop on the tongue and inside the mouth. They are usually round or oval, and can be white or yellowish with a red border. While the exact cause is unknown, they are thought to be triggered by minor injuries to the mouth, stress, hormonal changes, or a weakened immune system. They are generally harmless and heal on their own within a week or two.
Geographic Tongue
Geographic tongue is a harmless condition that causes patches on the tongue to appear smooth and red, resembling a map. These patches are not painful but may be slightly sensitive. The condition is believed to be related to inflammation and changes in the taste buds, possibly triggered by allergies, stress, or nutritional deficiencies. The appearance of the tongue can change over time. While harmless, it can be aesthetically concerning for some individuals.
- Appearance: Red and smooth patches that change location over time.
- Symptoms: Usually asymptomatic, but may have mild sensitivity.
- Treatment: No specific treatment is usually required; focus is on managing any associated symptoms.
Oral Thrush
Oral thrush is a fungal infection caused by an overgrowth of Candida yeast in the mouth. It causes white, creamy patches on the tongue and other areas of the mouth, which can be scraped off, leaving a red and sore underneath. This infection is more common in people with weakened immune systems, babies, or those who wear dentures. Oral thrush can be treated with antifungal medications prescribed by a doctor or dentist.
- Appearance: White, creamy patches that can be scraped off.
- Symptoms: Burning sensation, soreness, difficulty swallowing.
- Treatment: Antifungal medications (oral or topical).
Oral Lichen Planus
Oral lichen planus is a chronic inflammatory condition that affects the mucous membranes, including the tongue. It often appears as white or lace-like patches on the tongue and can cause burning, soreness, and sensitivity. The exact cause is unknown, but it is thought to be related to an autoimmune response. Oral lichen planus can be managed with corticosteroids or other medications to reduce inflammation, but it typically is a long-term condition.
- Appearance: White or lace-like patches, sometimes red and inflamed areas.
- Symptoms: Burning, soreness, sensitivity.
- Treatment: Corticosteroids, other anti-inflammatory medications, and supportive care.
Vitamin Deficiencies
Certain vitamin deficiencies, particularly B vitamins (like B12 and folate) and iron, can manifest as a sore tongue, often accompanied by other symptoms like fatigue, weakness, and pale skin. A sore tongue resulting from a deficiency may present with changes in color and texture, such as a smooth, red, or swollen tongue. Addressing the underlying deficiency through diet or supplements is crucial for resolving the sore tongue.
- Appearance: May appear smooth, red, swollen, or pale.
- Symptoms: Fatigue, weakness, pale skin (depending on the specific deficiency).
- Treatment: Dietary changes or supplements to correct the deficiency.
When should I see a doctor for a sore tongue?
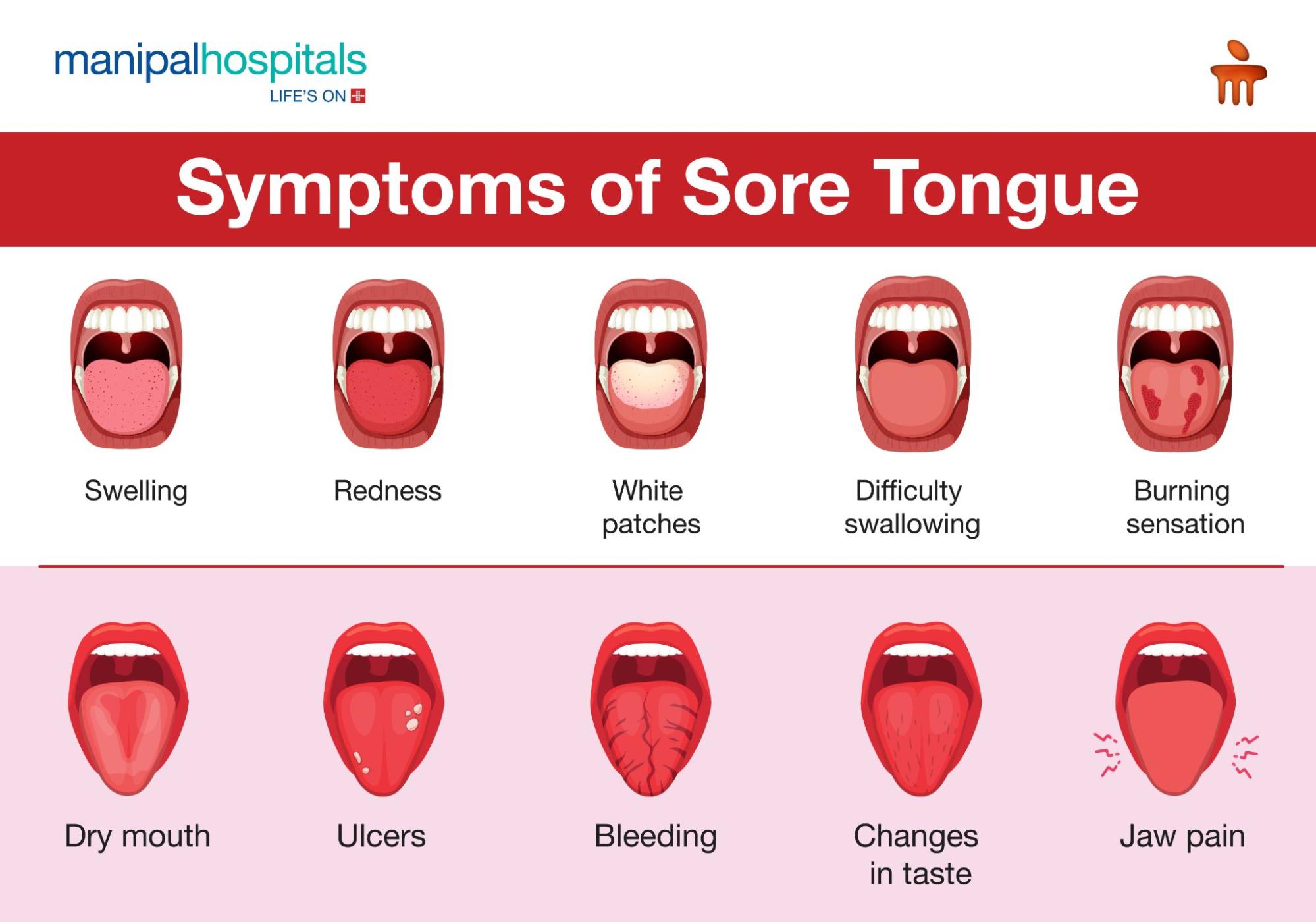
You should see a doctor for a sore tongue if the pain is severe, persistent, or accompanied by other concerning symptoms. A sore tongue, or glossitis, can be a symptom of various conditions, some minor and easily treatable, others more serious. Delaying treatment for a potentially serious underlying condition can lead to complications. Therefore, seeking medical attention is crucial when the discomfort becomes problematic or indicative of something more significant.
When the Soreness is Severe or Unrelenting
Persistent soreness that doesn't improve with home remedies like rinsing with salt water or applying a topical anesthetic should prompt a visit to the doctor. Intense pain that interferes with eating, drinking, or speaking warrants immediate attention. This could indicate a more serious underlying issue requiring medical intervention.
- Severe pain preventing normal eating and drinking.
- Persistent soreness lasting longer than two weeks despite home treatment.
- Pain that worsens progressively over time.
When the Sore Tongue is Accompanied by Other Symptoms
A sore tongue accompanied by other symptoms such as fever, swollen lymph nodes, difficulty swallowing, mouth sores, or a rash could indicate a more serious infection or underlying medical condition. These additional symptoms provide crucial clues for diagnosis and appropriate treatment. Do not hesitate to seek medical advice if you experience any of these alongside a sore tongue.
- Fever (high temperature).
- Swollen lymph nodes in the neck or jaw.
- Difficulty swallowing (dysphagia).
- Mouth sores (other than the sore tongue).
- Skin rash or other dermatological issues.
When You Have Risk Factors for Oral Cancer
Individuals with risk factors for oral cancer, such as smoking, excessive alcohol consumption, a history of HPV infection, or a family history of oral cancer, should seek medical attention for any persistent changes in their mouth, including a sore tongue. Early detection of oral cancer is vital for successful treatment. Even a seemingly minor sore tongue could warrant investigation.
- History of smoking or tobacco use.
- Excessive alcohol consumption.
- Human papillomavirus (HPV) infection.
- Family history of oral cancer.
If the Sore Tongue is Associated with Nutritional Deficiencies
A sore tongue can be a sign of certain vitamin deficiencies, such as vitamin B12 deficiency or iron deficiency anemia. If your sore tongue is accompanied by other symptoms suggestive of nutritional deficiencies, like fatigue, weakness, or pale skin, it's important to consult a doctor for testing and appropriate supplementation. Addressing the underlying deficiency is crucial for healing the sore tongue.
- Fatigue and unexplained tiredness.
- Weakness and muscle aches.
- Pale skin and other signs of anemia.
- Numbness or tingling in the extremities.
If Home Remedies Are Ineffective
If you've tried simple home remedies like rinsing your mouth with salt water or using over-the-counter pain relievers for several days, and the soreness persists or worsens, it's time to consult a doctor. This suggests the underlying cause may be more complex and require professional medical attention. Don't rely solely on home remedies for prolonged periods, especially if symptoms are severe or worsening. Seeking professional help is crucial when home care fails.
- Persistent soreness despite home treatment.
- Worsening symptoms after using home remedies.
- Lack of improvement after several days of self-care.
What deficiency causes a sore tongue?

A sore tongue, medically termed glossitis, can be caused by several nutritional deficiencies. The most common are deficiencies in iron, vitamin B12, and folate (vitamin B9). Other deficiencies, though less frequently the sole cause, can also contribute to or exacerbate a sore tongue. The symptoms can vary, ranging from a burning sensation and redness to swelling and changes in the tongue's texture. It's important to note that a sore tongue can also stem from other factors such as infections, allergies, or medications, so it's crucial to consult a healthcare professional for proper diagnosis and treatment.
Iron Deficiency Anemia and Sore Tongue
Iron deficiency anemia is a common cause of glossitis. Iron is crucial for the production of red blood cells, and a deficiency can lead to a pale, smooth, and sore tongue. This is because the tongue's papillae, the small bumps that give it its rough texture, atrophy due to lack of iron. The resulting smooth tongue can be painful and make eating difficult.
- Pale tongue: A characteristic sign of iron deficiency.
- Smooth tongue: Loss of papillae due to iron deficiency.
- Soreness and pain: Discomfort associated with the loss of papillae and inflammation.
Vitamin B12 Deficiency and Glossitis
Vitamin B12 is essential for nerve function and red blood cell production. A deficiency can lead to a variety of symptoms, including a sore, smooth, and often red tongue. This is because B12 plays a vital role in cell growth and repair, and its deficiency can disrupt the health and function of the tongue's tissues.
- Smooth, beefy red tongue: A characteristic sign of B12 deficiency.
- Burning sensation: Pain and discomfort experienced on the tongue.
- Numbness or tingling: Neurological symptoms associated with B12 deficiency.
Folate Deficiency and Oral Manifestations
Folate, or vitamin B9, is vital for cell growth and DNA synthesis. A folate deficiency can impact the rapid cell turnover in the mouth and tongue, resulting in a sore, inflamed tongue. Similar to B12 deficiency, it can manifest as glossitis, often appearing smooth and red.
- Inflammation and redness: Characteristic signs of folate deficiency.
- Soreness and pain: Discomfort associated with the inflammation.
- Potential for other oral lesions: Folate deficiency can also affect other parts of the mouth.
Riboflavin (Vitamin B2) Deficiency and Tongue Issues
While less commonly the sole cause of a sore tongue, riboflavin deficiency can contribute to glossitis. Riboflavin is involved in many metabolic processes, including those related to oral health. A deficiency can manifest as a sore, cracked, or inflamed tongue, often with a purplish hue.
- Cracked lips and corners of the mouth (angular cheilitis): Often seen alongside glossitis.
- Inflammation and redness of the tongue: Similar to other B vitamin deficiencies.
- Possible purplish discoloration: Distinctive from the pallor seen in iron deficiency.
Niacin (Vitamin B3) Deficiency and Pellagra
Severe niacin deficiency leads to pellagra, a condition characterized by the "three D's": dermatitis, diarrhea, and dementia. Glossitis is a common oral manifestation of pellagra. The tongue may appear inflamed, red, and swollen. In advanced cases, the tongue can become ulcerated and severely painful.
- Inflammation and redness: Similar to other B vitamin deficiencies.
- Swelling and ulceration: Can be severe in advanced pellagra.
- Systemic symptoms: Dermatitis, diarrhea, and dementia are key characteristics of pellagra.
What diseases cause tongue pain?

What Diseases Cause Tongue Pain?
Tongue pain, or glossodynia, can stem from various underlying medical conditions. It's important to note that the pain can manifest in different ways, from a burning sensation to sharp, stabbing pains. The location and nature of the pain can often provide clues to the underlying cause. Accurate diagnosis requires a thorough examination by a healthcare professional to rule out serious conditions and develop an appropriate treatment plan. Self-treating can be dangerous, and prompt medical attention is advised if experiencing persistent or severe tongue pain.
Infections
Infections are a common cause of tongue pain. Viral infections like the common cold or flu can sometimes cause inflammation and soreness of the tongue. Bacterial infections, such as strep throat, can also lead to tongue pain, often accompanied by other symptoms like a sore throat and fever. Fungal infections, particularly oral thrush (candidiasis), are frequent culprits, especially in individuals with weakened immune systems. These infections can create a white or yellowish coating on the tongue, accompanied by burning or soreness.
- Viral Infections: Common cold, flu, resulting in inflammation and soreness.
- Bacterial Infections: Strep throat, leading to tongue pain, sore throat, and fever.
- Fungal Infections: Oral thrush (candidiasis), causing white/yellow coating, burning, and soreness. Often seen in immunocompromised individuals.
Oral Health Issues
Poor oral hygiene practices can contribute to various conditions leading to tongue pain. Gingivitis and periodontitis (gum disease) can indirectly affect the tongue through inflammation and irritation. Dental abscesses can also cause referred pain to the tongue. Additionally, trauma to the tongue from biting or accidental injury can cause significant pain and swelling. Regular brushing, flossing, and dental checkups are vital in preventing these issues.
- Gingivitis/Periodontitis: Gum disease leading to tongue irritation through inflammation.
- Dental Abscesses: Infection causing referred pain to the tongue.
- Trauma: Biting or injury to the tongue, resulting in pain and swelling.
Nutritional Deficiencies
Certain vitamin and mineral deficiencies can manifest as tongue pain. A deficiency in vitamin B12, iron, or folic acid can lead to glossitis, an inflammation of the tongue, which is characterized by soreness, redness, and swelling. These deficiencies often have other associated symptoms, such as fatigue, weakness, and anemia. A balanced diet or supplementation under medical supervision can help address these deficiencies.
- Vitamin B12 Deficiency: Causes glossitis (inflammation), soreness, redness, swelling.
- Iron Deficiency: Contributes to glossitis and overall fatigue.
- Folic Acid Deficiency: Similar to B12 deficiency, leading to glossitis and other systemic symptoms.
Autoimmune Diseases
Autoimmune diseases, where the body's immune system attacks its own tissues, can cause tongue pain. Sjögren's syndrome, an autoimmune disorder affecting the moisture-producing glands, can lead to dry mouth and a burning sensation on the tongue. Lupus, another autoimmune disease, can cause inflammation and pain in various parts of the body, including the tongue. Diagnosis and management of these conditions require specialist care.
- Sjögren's Syndrome: Dry mouth and burning tongue sensation.
- Lupus: Inflammation and pain in various parts of the body, including the tongue.
- Other autoimmune diseases: Can also manifest with tongue pain as a symptom.
Allergic Reactions
Allergic reactions to certain foods, medications, or oral hygiene products can trigger tongue pain. The reaction might present as swelling (angioedema), itching, or a burning sensation. Contact allergy from ingredients in toothpaste, mouthwash, or dental materials can also cause localized tongue irritation and pain. Identifying and avoiding the allergen is key in managing this type of tongue pain. In severe cases, immediate medical attention is necessary.
- Food Allergies: Swelling, itching, burning sensation.
- Medication Allergies: Similar symptoms to food allergies.
- Contact Allergies (e.g., toothpaste, mouthwash): Localized tongue irritation and pain.
What causes a sore tongue?
A sore tongue, medically known as glossitis, can stem from a variety of causes. One common culprit is oral thrush, a fungal infection caused by Candida albicans. This often presents as a white or creamy coating on the tongue, accompanied by soreness and burning. Nutritional deficiencies, particularly in iron, vitamin B12, and folic acid, can also lead to a sore tongue. These deficiencies can affect the tongue's health, causing it to become inflamed and painful. Allergies to certain foods or oral hygiene products can trigger an allergic reaction, manifesting as a sore and irritated tongue. Similarly, medications, such as chemotherapy drugs or antibiotics, can have a side effect of glossitis. The medication alters the natural bacterial balance in the mouth, creating an environment conducive to irritation or infection. Certain medical conditions like geographic tongue (benign inflammatory condition), and lichen planus (chronic inflammatory disease) can also cause a sore tongue. Finally, mechanical irritation from sharp teeth, ill-fitting dentures, or even habitually biting the tongue, can cause trauma and subsequent soreness. Therefore, a sore tongue is often a symptom, not a disease itself, requiring investigation into the underlying cause.
Is a sore tongue a serious symptom?
While a sore tongue is not always a sign of a serious condition, it's crucial to not dismiss it entirely. In many cases, a sore tongue is a relatively minor issue caused by something easily treatable like a minor infection or irritation. However, a persistent or worsening sore tongue, especially accompanied by other symptoms like fever, difficulty swallowing, or unexplained weight loss, could indicate a more serious underlying medical problem. Conditions such as cancer (oral cancers, such as squamous cell carcinoma), severe vitamin deficiencies leading to anemia, or certain autoimmune diseases can manifest with a sore tongue as one of the symptoms. Therefore, if your sore tongue is accompanied by other concerning symptoms, or if it persists despite home remedies or over-the-counter treatments for several days to weeks, it is essential to seek medical attention for proper diagnosis and treatment. The earlier a serious condition is diagnosed, the more effective the treatment is likely to be.
When should I see a doctor about a sore tongue?
You should consult a doctor if your sore tongue persists for more than two weeks despite trying home remedies like rinsing your mouth with salt water or using a soothing mouthwash. Additionally, if the soreness is accompanied by other symptoms such as fever, difficulty swallowing, bleeding from the tongue, unexplained weight loss, mouth sores, or difficulty speaking, you should seek immediate medical attention. A sore tongue accompanied by white patches or a thick coating might suggest an oral fungal infection that requires medical intervention. Similarly, if the soreness is severe and interferes with your ability to eat, drink, or speak normally, it's best to consult a doctor. Finally, if you have risk factors for oral cancer, such as smoking, excessive alcohol consumption, or a family history of oral cancer, any persistent changes in your mouth, including a sore tongue, should be promptly evaluated by a healthcare professional.
What are the treatment options for a sore tongue?
Treatment for a sore tongue depends entirely on the underlying cause. If the soreness is due to a fungal infection like oral thrush, your doctor may prescribe an antifungal medication, either topical or oral, to clear the infection. For nutritional deficiencies, your doctor will likely recommend dietary changes or vitamin supplements to correct the imbalance. If the cause is an allergy, identifying and avoiding the allergen is key. This could involve switching oral hygiene products or eliminating certain foods from your diet. In cases of mechanical irritation, adjustments might be necessary, such as getting dental work to correct sharp teeth or ill-fitting dentures. For more serious conditions such as autoimmune diseases or cancers, specific treatment plans will be developed based on the diagnosis. These could include medications, therapies, and possibly surgery. Pain relief can be achieved through over-the-counter pain relievers like ibuprofen or acetaminophen, and mouthwashes containing lidocaine can provide temporary relief from pain and discomfort. However, self-treating can delay proper diagnosis, so consulting a medical professional for a proper diagnosis is crucial to determine the right treatment plan.
Deja una respuesta